Brain Tumors
Key Points
- One of California's Largest Brain Tumor Centers
- The most complex brain tumors that are thought to be inoperable are removed with lengthy meticulous surgery
- Neurophysiological monitoring of infants and young children allows brain function to be monitored during brain tumor surgery
- Head Start Chemotherapy Protocols to cure malignant brain tumors without radiation
- Laser surgery for tumor removal
What is a Brain Tumor?
A tumor means that a part of the body has grown out of control. There are low grade brain tumors and high grade malignant brain tumors.
Low grade tumors mean that the type of cell that makes up the tumor is not likely to grow out of control and spread to remote parts of the brain. Surgery for low grade tumors can often be curative. However, low grade tumors can grow and send roots into a critical part of the brain that is essential for the normal functioning in a child's life. When the “roots” are shallow, careful, meticulous dissection can still remove the tumor. If the “roots” are too deep into critical areas of the brain, chemotherapy may be needed in conjunction with surgery to cure these low grade tumors.
High grade, malignant brain tumors, otherwise known as brain cancer, represent cells that have grown out of control. They run the risk of not only causing damage in the area right around the tumor, but can also spread to other parts of the brain (metastases). Malignant brain tumors may also spread to other parts of the body. There are many different types of malignant brain tumors. The type depends on the cell type from which the tumor originated. The naming of tumors can include the name of the cell type and its location. Surgery is important to remove as much of the tumor as possible. Chemotherapy can then kill the remaining cells. In older children, radiation may also be required
Brain cancer accounts for 15% of pediatric cancers. Over 60% of brain tumors occur in the lower region of the brain called the posterior fossa. The remaining brain tumors occur in one of the two cerebral hemispheres or in the spinal cord.
The naming of brain tumors is complex. Many Internet sites exist to help people understand the names used for the cancers, and also describe the cancers in more detail. A list of links explaining several different types of brain cancers is in the right hand column of this page.
Common Brain Tumor Names
Brain tumors are named by cell type, (i.e. histology). Common brain tumors include primitive neurectodermal cells, glioma, astrocytoma, ependymoma. Tumors like PNET( Primitive Neuroectodermal Tissue) and ependymomas are high grade or malignant brain tumors. Tumors like astrocytomas and gliomas can be high grade or low grade.
Brain tumors are also classified by location: cerebrum, cerebellum, brain stem, pons, midbrain and the optical nerve. Location of a tumor can have biological implications. The pons tumors are usually high grade, while midbrain tumors are usually low grade. So, the name used to describe a brain tumor can involve both the cell type from which the cancer arose and the location of the cancer. An example of this would be “cerebellar astrocytoma”. “Cerebellar” means the cancer is in the cerebellum. “Astrocytoma” means that the tumor cells came from astrocytes, which are star shaped cells and are part of the supportive tissue of the neurons. Another example of this is “brain stem glioma”. “Brain stem” means that the tumor originated in the brain stem. “Glioma” means the tumor came from glial cells, which are supportive tissues of the brain.
Diagnosis of Brain Tumors
Brain Tumor Symptoms
The brain has many functions, but the brain itself has no sensation of pain. Because of this, the symptoms of a brain tumor can be quite varied. Many of the symptoms can act like other minor disorders. This is important to know, because many parents feel guilty about not recognizing that something serious was going on with their child. Often times, it is difficult to diagnose brain tumors when the symptoms mimic other less serious disorders, particularly in young children who may not yet be verbal.
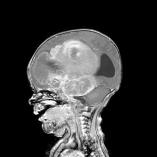
The symptoms usually depend on the type of tumor and where it is in the brain. Because the brain itself does not perceive pain, a tumor can reach enormous size and cause extra pressure within the skull (called increased intracranial pressure). Stretching of the skull and its coverings cause headaches, decreased attention and vomiting. The tumor can sometimes cause hydrocephalus, which is a blockage of cerebrospinal fluid flow, causing extra brain pressure. Extra brain pressure can cause a host of symptoms, including headaches (usually early morning) combined with nausea or vomiting, poor coordination, drowsiness, and a decrease in school performance. Additionally, in children and teens, symptoms can include weakness in a limb or one side of the body, speech problems, balance problems, limb tingling, or loss of bowel and bladder control. In babies, symptoms are less obvious than in children and teens, and may include loss of coordination, missed milestones, weakness in a limb or on one side of the body, or an abnormally rapid increase in head size and full fontanelle.
If your doctor suspects a brain tumor, pictures of the brain are usually taken, and this can be done by a computed tomography (CT) scan, or magnetic resonance imaging (MRI), or both. A CT scan or MRI may be done with an injection of dye in the vein that will enhance the machine's ability to see the tumor. The brain picture will be read by a radiologist. The radiologist may have an idea of what type of brain tumor is present by the location and the way the images look. However, the only way to really know what type of brain tumor is present is to have a pathologist study it under a microscope.
Once a final diagnosis is made, usually 5-10 days after surgery, a team of doctors will meet and determine the right treatment for your child. The team includes a neurosurgeon, radiologist, neuro-oncologist, and neuropsychologist, and a social worker
Brain Tumor Treatments
Brain Tumor Surgery
Surgery plays a critical role in most brain tumors. Low grade tumors that are completely removed, or resected, can be cured without additional treatment. For those low grade tumors that that send deep roots into vital parts of the brain that cannot be removed, resecting as much of the tumor as possible without affecting the vital parts of the brain allows chemotherapy to work on the smallest amount of cells. In malignant tumors, removing the tumor also set the stage for a cure by chemotherapy or radiation to treat the least amount of cancer cells. In a brain cancer such as ependymoma, resecting all or nearly all of the tumor can offer the best chance of a cure. Sometimes a tumor cannot be resected at all because of its location and diffuse nature intertwining with critical parts of the brain. In this case surgery is performed to obtain a small piece, (or biopsy of the tumor) to determine what kind of tumor it is.
New technology continues to improve the neurosurgeon’s ability to remove previously inoperable tumors with less risk from surgery. We utilize a microscope, computer guidance, and an intraoperative ultrasound and CT to guide the surgery. In addition, we always monitor the nerve and brain functions even as the patient is under anesthesia. This is to make sure that surgery is not affecting normal functions. Most importantly, the surgeons make all the difference. We are dedicated to removing all of the tumor in a safe fashion. The length of a surgery can be quite long for a complex tumor. A brain surgery of 12 plus hours is quite routine in our hospital.
Brain Tumor Radiation
Radiation therapy involves aiming high energy directly at the tumor, thus killing the tumor cells. This high energy is in the form of x-ray radiation or gamma rays. Radiation therapy may harm normal tissue near the tumor or along the path of the energy beam,The most important side effect is the long-term cognitive decline in children who have major areas of the brain radiated. Children under three years of age pose a particular problem because their brains are still undergoing a great deal of development. Thus, radiation therapy is usually not considered as an option for these young children.
Therefore, radiation therapy is mostly reserved for malignant brain tumors in older children. However, on rare occasions, some benign tumors are considered treatable with radiation therapy if their location is considered to be too dangerous to remove with surgery. With chemotherapy and surgery, however, our team has not been required to use radiation for lower grade tumors for many years.
Because children must be absolutely still during treatment, many are sedated or are treated with anesthesia for the radiation treatments.
New technologies are constantly being developed to improve the destruction of tumor cells, to reduce the damage to normal brain tissue, and to reduce the overall side effects of radiation therapy. One example of this is IMRT (Intensity Modulated Radiation Therapy) where radiation is calculated from many beams to reduce the harm to any one. Another is radiosurgery (Gamma Knife), where the head is positioned and steadied in a metal ring and a single dose of radiation is given from a modified linear accelerator to burn a 1 inch hole in a precise part of the brain. The limitation of radiosurgery is the size of the tumor it can treat (less than one inch). It does not kill the tumor outside of the one inch margin, and it can harm critical structures adjacent to the target.
Brain Tumor Chemotherapy
Chemotherapy is the use of certain drugs that try to kill or slow down the growth of tumor cells. These drugs are usually used after surgery to kill off the tumor cells left behind. Unlike radiation therapy, normal brain tissue is not significantly affected. However, because most chemotherapy drugs are given through the vein, other parts of the body outside the brain can be affected as a side effect of the treatment.
The types of drugs used, how they are given, and the schedule of giving them are determined by the neuro-oncology team, and depend on the location and type of tumor, as well as on the age of the patient. This is called a “protocol”. Treatment is usually a series of monthly infusions for up to a year.
Some of the drugs can be given by mouth, either as a pill or liquid. However, most of the drugs are given through the vein. When the chemotherapy is scheduled to be given over a long period of time, if the child has small veins or difficult to access veins, a larger catheter may be placed in a major vein for the duration of drug treatment.
Innovations in chemotherapy treatment of malignant brain tumors
Over the past 30 years we have made tremendous strides in the United States in the treatment of children with malignant brain tumors. One of the most significant advances, however, has been the appreciation of the tremendous negative impact that radiation therapy delivered to the whole brain can have on the intellectual development of children. We also realize that aggressive chemotherapy can, in many instances reduce or eliminate the need for such treatment, especially in the youngest of children.
What is the Head Start Consortium?
For the past five years the Neuro-Oncology Program at Children’s Hospital & Research Center Oakland has participated in the Head Start Consortium. This group of 42 pediatric brain tumor centers in the US, Canada and abroad have banded together to develop new strategies for the treatment of malignant brain tumors in children. The goal is to achieve cure rates equivalent to those seen with traditional therapy while avoiding, as much as possible, the devastating effects of radiation therapy on the developing brain. Since the first Head Start study began in 1991, over 200 children have been treated using this approach, which involves 4-5 courses of intensive but conventional chemotherapy followed by a single course of extremely high dose, marrow destructive chemotherapy (the equivalent of receiving one year of drug treatment in six days). This is followed by “rescue” with infusion of the child’s own blood stem cells. No radiation therapy is given to children less than 6 years of age at diagnosis unless the tumor is still seen on an MRI. This scan is done just prior to their receiving the high dose chemotherapy.
The results from Head Start II demonstrate that over 70% of children less than 6 years of age whose tumors were completely removed at the time of diagnosis and who have no evidence of spread of tumor elsewhere can be cured of their tumor without the use of radiation therapy. Careful examination of IQ and brain function many years after completion of therapy has revealed no loss of brain function in these children when compared to testing performed after completion of their chemotherapy. This is very different than the pattern seen in young children treated with radiation therapy, who predictably lose 20 IQ points or more following whole brain radiation.
We anticipate that with Head Start IV, we will see further improvements in the cure rates for these aggressive brain cancers, while continuing to preserve the cognitive functioning of our patients to the greatest extent possible.



